COVID-19 Updates
Here's What We Know
Payer Updates Change Frequently.
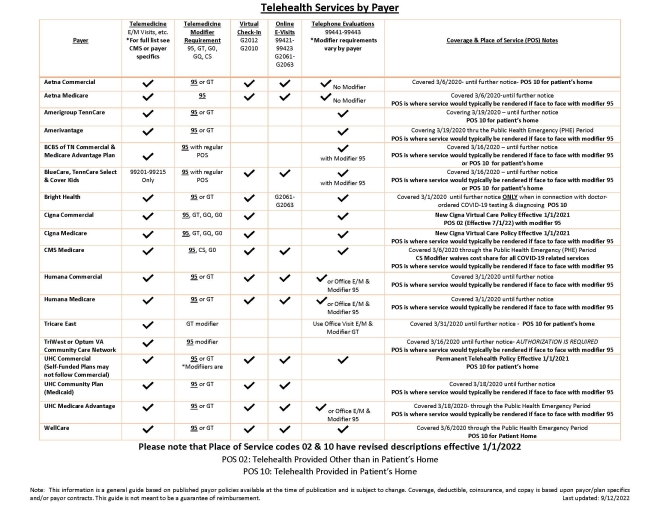
Stay current on policy updates to receive proper reimbursement for telehealth services. UPA has added general guidance from payers for patient cost-sharing to our telehealth services grid below to help ensure appropriate balancing billing and copay collection for patients. Payer policies and additional resources can be found below in our Payer Source Documents section.
The Telehealth Services by Payer details provided below is current as of its publication date of 9/12/2022 and is subject to change.
COVID-19 Payor Source Documents
Aetna

|
Click to view: 2/8/21 Update
Click to view: 7/7/20 Update
Click to view: 4/21/20 Update
Click to view: 3/31/20 Telemedicine Policy
3/26/20
COVID-19: Taking Action
Dear Valued Partner:
We share the same goal: help people get and stay healthy. We’re your partners in health care, and act to serve you and the millions of patients who rely on us for their health care needs.
In response to the rapidly evolving COVID-19 outbreak, CVS Health and Aetna are here to support you with timely answers and information. Through CVS Health and Aetna’s combined resources and your partnership, we can best support your Aetna patients’ health and well-being, ensure their access to medication and remove barriers to care.
We’re here to help you, help your patients and recently announced these resources and enhancements when applicable:
If you request testing related to COVID-19,we’ll waive your Aetna patient’s cost sharing.
Aetna Commercial patients pay for covered telemedicine visits until June 4, 2020.
Until further notice, Aetna is also expanding coverage of telemedicine visits to its Aetna Medicare members, so they can receive the care they need from you without leaving their homes.With this change and new flexibilities announced by the Centers for Medicare and Medicaid Services to help combat the virus, Aetna Medicare members can now see their providers virtually via telephone or video.
Aetna is offering its Medicare Advantage brief virtual check-in and remote evaluation benefits to all Aetna Commercial members and waiving the co-pay.
Care packages will be sent to Aetna patients diagnosed with COVID-19. Through Aetna’s Healing Better program, Aetna Commercial and Medicare Advantage members will receive CVS items to help relieve symptoms as well as personal and household cleaning supplies to help keep others in the home protected from potential exposure. Call the number on your Aetna patient’s ID card to register a recently diagnosed patient.
Patients won’t have to pay a fee for home delivery of prescription medications from CVS Pharmacy®.
We’re waiving early refill limits on 30-day prescription maintenance medications for all Commercial members with pharmacy benefits administered through CVS Caremark.
Aetna Medicare members may request early refills on 90-day prescription maintenance medications at retail or mail pharmacies if needed. For drugs on a specialty tier, we’re waiving early refill limits for a 30-day supply.
Through existing care management programs, Aetna will proactively reach out to your patients who are most at-risk for COVID-19.
Please refer to the “What You Need to Know About the Coronavirus (COVID-19) - Aetna Providers” FAQs on Aetna.com for additional important information. There, you’ll find information about codes related to COVID-19 and selected labs approved to do COVID-19 testing. This page will continually be updated with information as it becomes available to help you care for your patients.
Let’s work together to provide your patients with a clear path to care. Thank you for your continued partnership.
Best Regards,
Angie Meoli
SVP, Network Strategy and Provider Experience
AMA
|
|
|
|
|
BREAKING NEWS: AMA announces new CPT® codes for multi-virus tests to detect COVID-19 and flu |
|
The American Medical Association (AMA) published an update to the Current Procedural Terminology (CPT®) code set that includes new code additions and editorial revisions for reporting medical services. |
|
For quick reference, the two new Category I CPT code and descriptors are: |
|
87636
|
|
CPT codes ranging from 87301 to 87430 were also revised by removing the undefined term “multi step method” from code descriptors. The revision clarifies the proper reporting for antigen tests that are read by a machine, as compared to those which can be visually interpreted without a machine. |
|
87426
|
|
In accordance with the above revision, the CPT Editorial Panel approved a new category I code, 87811, to report infectious agent antigen detection by immunoassay with direct visual observation. |
|
87811
|
|
In addition to the long descriptors, short and medium descriptors for CPT codes 87636, 87637, 87426 and 87811 can be accessed on the AMA website, along with several other recent modifications to the CPT code set. |
|
For more information you can see the press release
here.
|
|
CPT © Copyright 2020 American Medical Association. All rights reserved. AMA and CPT are registered trademarks of the American Medical Association. |
|
American Medical Association |
|
On September 8, 2020 the AMA released two new COVID related CPT codes for immediate use.
Reference link to the following AMA Article for more details: https://www.ama-assn.org/practice-management/cpt/covid-19-coding-and-guidance?gclid=EAIaIQobChMIvPPH8-vr6wIVx8DACh0W3gBREAAYASAAEgL0tvD_BwE Reference link for AAPC Article Blog post: https://www.aapc.com/blog/51794-ama-approves-2-new-cpt-codes-for-covid-19/ |
Amerigroup
Click to view July 2021
View September 17, 2020
July 27, 2020
Dear Episodes of Care Provider,
In light of the additional burden of caring for our TennCare members during this pandemic, TennCare has decided to waive all 2019 risk-sharing payments for the Episodes program. This news has also been posted to the TennCare website under “News and Announcements” or you can follow this link: TennCare Memo: Waiving 2019 Episodes Risk-Sharing Payments.
Providers in gain-share on their final 2019 reports will still receive those payments.
Please note the following:
- Final reports for 2019 AND Quarter 1 reports for 2020 will be out on August 21st. Please use these reports to see how you are trending. You will be notified by email when the reports are posted.
- No action is required by providers in the risk-share group. You will still see the same data on the final reports but you will not be asked to submit a risk-share payment. Please take advantage of this report to impact your 2020 reports.
- Providers who have a net gain-sharing payment across all episode types in their final 2019 performance report will receive those payments as planned, with no changes. This means that providers will have any risk-sharing amounts subtracted from their total gain-share to find their net gain-sharing amount. This is the same calculation that occurs every year to calculate a provider’s net gain- or risk-sharing amount.
- Your Amerigroup team is eager and available to have a webex with your practice. We can review reports, offer provider education, and provide coaching on how to do well with the Episodes Initiative.
- Reply to this email with requests or questions for your Amerigroup team.
- TennCare is still analyzing the impact of the pandemic on the 2020 performance period and is open to input from stakeholders. You may provide feedback or suggestions to TennCare by e-mailing the state at Payment.Reform@tn.gov.
Be watching for your notification for your next reports on August 21st.
And we sincerely thank you for your excellent care of your patients during these unprecedented times.
Julie Riedel, APRN, Family Nurse Practitioner
Provider Clinical Liaison
22 Century Blvd., Suite 220, Nashville, TN 37214
O: (615) 316-2400 x 106-126-0154| M: (615) 806-4283
AGPEpisode.Reporting@Amerigroup.com

June 9, 2020
Click to view: Amerigroup Tenncare Telehealth Coverage Policy
June 5, 2020
Click to view: Amerigroup Medicare Advantage Telehealth Coverage Policy FAQ
June 2020
Click to view: Amerigroup Medicare Advantage Memo 6/17/2020
May 2020
Click to view: Amerigroup Medicare Advantage
BCBS

Click to view BlueCare Telehealth 7.2021
Click to view BCBST Provider FAQ 7.2.20
Click to view BCBST Provider FAQ 6.17.2020
Click to view BCBSTN FAQ 5.18.20
Click to view BCBS Telehealth Update 5.14.20
Click to view BCBS FAQ 4.24.20
Click to view BCBS FAQ 4.21.20
Click to view BCBS 4.7.20 UPDATES
Click to view BCBS 4.2.20 FAQ
Click to view PCP Lock-in Requirements
Click to view updated FAQ 3/26/20:
Click to view the documents:
BrightHealth
Click to view: Telehealth eMail 4.3.20
Click to view: DoctorOnDemand 4.3.20
Click to view: Bright 3.19.20 Utilization
Click to view: Bright 3.27.20 Claims
Cigna

Click to view 10/7/21
Click to view 4/8/21
Click to view vaccine hesitancy
Cigna Commercial Virtual Care Policy
2.8.21
Dec 2020
Virtual Care Policy
Nov 2020
Inject / Non-inject
11.20.20
Oct 2020
Virtual Care Policy
7.24.20
7.23.20
7.16.20
Click to view update 7.16.20
5.22.20 Update
Click to view 5.22.20 Update
5.13.20 Medicare Advantage Guidelines
Click to view Cigna Medicare Advantage Guidelines
5.11.20 Update
Click to view 5.11.20 Update
Referral Guidelines
Click to view Cigna Referral Guidelines
4.24.20 Update
FAQ 4.13.20
Click to view Cigna 4.13.20 FAQ
Interim Virtual Care Billing Guidelines (3/30/20):
Click to view 3/30/20 Interim Virtual Care Billing Guidelines
3/27/20:
Cigna has released new Telehealth guidelines to expand covered services.
Click the logobelow to view this document:
3/24/20 Data:
PCP referrals for specialist office visits are being waived temporarily until May 31st, effective immediately, for SureFit and IFP Connect Network customers in response to the COVID-19 virus outbreak. Suspending the referral requirement will allow our providers and Clinical Intake teams to focus on COVID-19 critical care needs during this time, such as ER and Urgent admission authorizations.
- Continue to follow all other processes as outlined in your summary plan description (e.g. Authorizations are still required)
- Given this is a fluid situation the possibility of extending beyond the May 31st date will be evaluated on an ongoing basis.
Your claims will not be denied without a referral.
We’ve had several providers ask if Physical Therapy could be performed virtually and below are the updates around PT.
Q: Will Cigna temporarily expand coverage of benefits for physical therapy to include virtual care?
A: Yes. There are 2 scenarios:
-A homecare agency that traditionally has provided PT services in the home does them via telehealth and bills “G” codes that will pay according to the fee schedule.
-An traditionally outpatient PT clinic performs PT services in the home via telehealth and bills E&M codes will pay according to their fee schedule
Q: Will Cigna temporarily expand coverage of benefits for physical therapy to allow in network providers to provide care in home as alternative to “in center” traditional therapy services?
A: No. Face-To-Face services in the home are the purview of Carecentrix and homecare agencies.
Click to view Cigna link 3/24/20: Cigna Makes It Easier For Hospitals To Focus On COVID-19 By Helping Accelerate Patient Transfers
CMS
UPDATED DOCUMENT April 3, 2020
Click to view the UPDATED Telehealth Waiver 1135 4.3.20
Click to view: MLN 4.3.20
Click to view: CMS update 4.1.20
Click to view: CMS update
Click to view: CMS Trump 3.31.20
Click to view CMS Update 3.31.20
Click to view CMS Covid19 Update 3/30/20
Click to view: Emerg Declaration Fact Sheet 3-13-20
Click to view: CMS Medicare Telemedicine 3-17-20
Click to view: MLN Telehealth
Humana

Click to view TeleHealth 7.28.01
Click to view 12.4.20
Click to view TeleH Updates 5.21.20
Click to view TeleH updates 5.1.20
Click to view updates for FAQ 5.1.20
Click to view Update 4.13.20 FAQs
Click to view 4.1.20 FAQ
Click to view updated FAQ 3/30/20
Click to view documents below
Click to view 3/23/20 Provider News
Click to view 3/23/20 Telehealth Humana
Click to view documents:
Humana Website Reference:
https://www.humana.com/provider/coronavirus
https://www.humana.com/coronavirus/covid19-humana-member-resources
Intergy Support
The UPA Intergy Support team continues to be available by both email and phone. As things change, we may experience higher call volumes and/or we may transition to working from home as need dictates.
If you cal